Infectious diseases are those that originate from the environment, and are transmitted from one living being to another through direct or
indirect contact. Infectious diseases may be caused by viruses, parasites/protozoa or bacteria. They may be spread through airborne dust, in water or feed contamination, close contact with neighboring livestock, other animals or wildlife. Some are spread by contact with infected blood, carried by vectors like flies, mosquitoes or ticks, syringes or veterinary instruments. See Biosecurity to read more about prevention using closed herds and quarantine.
Table No. 1 lists infectious diseases that most North American cattle can (should?) be tested for. If you breed cattle and export frozen genetics to the European Union, the list would be longer.
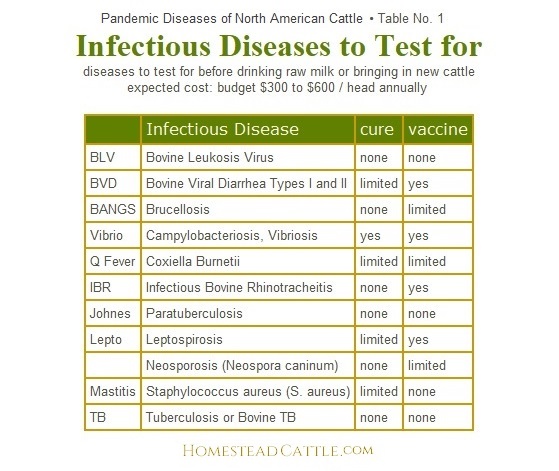
Once introduced on the farm, most contagious viral infections cannot be cured. It is easier on cattle and the farm budget to prevent disease rather than treat it. Many common viral diseases may be prevented with vaccination. Although the issue can be argued, the USDA National Organic Program (NOP) not only approves of vaccination, but strongly recommends it, especially for open herds. Table 2 lists the most commonly recommended core vaccines for cattle herds in North America:
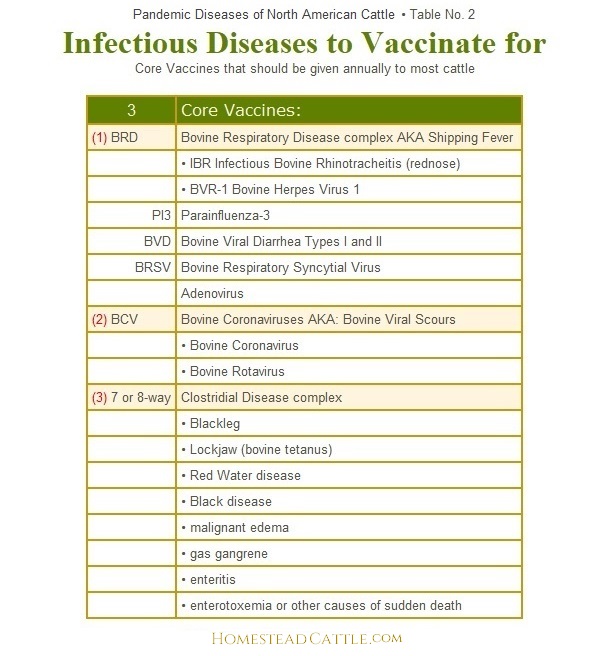
Alphabetic List of
Infectious Diseases
of North American Cattle
Pandemic diseases, listed in the tables above, are the most prevalent, widespread and problematic diseases in North American cattle.
Endemic diseases are situational, localized or regional infectious diseases. Risks for endemic cattle diseases will vary by region, season, climate or other factors. All the major infectious diseases in North American cattle are listed below in alphabetic order, with more detailed information about their prevention, vaccines, symptoms, and treatment.

Anaplasmosis is an infectious blood disease in cattle caused by a parasitic bacteria
that lives inside Red Blood Cells. It is also known as yellow-bag or
yellow-fever. Anaplasma marginale is a rickesttsial parasite that
causes Anaplasmosis in North America. It occurs primarily in warm, tropical
and subtropical areas. The disease is transmitted most commonly by ticks,
biting flies, by contaminated needles, dehorning equipment, castrating
knives and tattoo instruments. Mechanical transmission happens in just
minutes, as these blood parasites do not survive outside the host animal
longer than that. This intracellular parasite destroys RBCs, causing
anemia, fever, weight loss, breathlessness, uncoordinated movements,
abortion and death. Diagnosis is based on clinical signs and the examination
of blood under microscope for evidence of the parasite. Affected cattle
either die or begin a recovery within 4 days after the first signs of
the disease. The mortality rate increases with the age of the animal
when affected. Unless infected cattle are detected during the early
stages of the disease they should not be treated. If an animal with
advanced anaplasmosis is treated, it can actually die from lack of oxygen
from the stress of treatment. Animals that are infected and recover,
become carriers and will spread the disease. Carrier animals can sometimes
be cleared of anaplasmosis with repeated injections of long-acting oxytetracycline
(ex. LA-200®) or prolonged feeding of chlortetracycline.
Anthrax,
is another "sudden death" syndrome disease. It occurs worldwide
and is usually discovered with sudden death of cattle and sheep. Anthrax
can infect all warm-blooded animals, including humans. The anthrax organism
(Bacillus anthracis) has the ability to form spores which are resistant
to adverse conditions. Pasteurization or ordinary disinfectants may
destroy anthrax organisms in animals or their secretions. However, if
the infected animal carcass is opened and the organisms are exposed
to air, the bacilli will form spores. Sporulated anthrax organisms are
highly resistant to heat, cold, chemical disinfectants and drying. The
anthrax spore can live up to 5 years in surface soil and indefinitely
in deep soils. Anthrax is highly fatal and treating infected animals
is difficult. Penicillin is the antibiotic of choice. An effective vaccine
is available. Because anthrax is a reportable disease, details on the
use of the vaccine should be coordinated through the office of the state
veterinarian.
Bloat is prevented by
proper management, and culling genetically susceptible cattle. Bloat is caused by
an inherited tendency for bloat, exacerbated by certain proteins in
forage (particularly in legumes), the coarseness of the roughage and
the type of rumen microbial population. Pasture bloat usually occurs
in animals grazing lush legumes (alfalfa, clover) or wheat pasture.
To prevent pasture bloat in cattle you should plant pastures so that
no more than 50 percent of the forage mixture is alfalfa or clover.
Fill cattle on dry roughage or grass pastures before turning them into
legume pastures, and provide grass hay or graze in a rotation using
grass pastures. Visual signs of bloated cattle include distension of
the left side of the animal, discomfort (indicated by stomping of feet
or kicking of belly), labored breathing, frequent urination and defecation,
and sudden collapse. 
Bluetongue Virus (BTV): is a non-contagious infectious disease usually
transmitted by biting insects. Most bluetongue infections in cattle
are subclinical--but cattle comprise the main reservoir of BTV virus.
With exposure, sheep are the usual victims of bluetongue. In the U.S.,
the principal vectors are C. sonorensis and C. insignis, which are most
common in southern and western regions of the U.S. Sheep as well as
White-tailed deer, Pronghorn antelope and Desert Bighorn sheep are susceptible
to BTV infection. Bluetongue is of interest to APHIS because when it
occurs in domestic animals, it must be reported to the World Organization
for Animal Health (OIE). At least 26 serotypes of BTV have been identified
worldwide. 13 serotypes (1, 2, 3, 5, 6, 10, 11, 13, 14, 17, 19, 22,
and 24) have been reported in the US, with only types 2, 10, 11, 13,
17 considered endemic (a disease that occurs regularly in a particular
area). The only vaccine approved for BTV is a modified-live vaccine
that protects only against serotype 10.
Bovine Coronaviruses (BCV) cause respiratory and enteric infections in cattle and wild ruminants. AKA: Bovine Viral Scours — Bovine Winter Dysentry — Coronaviral Enteritis of Calves — Scours — Winter Dysentery. BCV is a pneumoenteric virus that infects the upper and lower respiratory tract and intestine. BCV is the cause of 3 distinct clinical syndromes in cattle: (1) calf diarrhea, (2) winter dysentery with hemorrhagic diarrhea in adults, and (3) respiratory infections in cattle of various ages including the bovine respiratory disease complex or shipping fever of feedlot cattle. It is shed in feces and nasal secretions and also infects the lung. The Veterinary Clinics of North America. Food Animal Practice, published online 2010 Jul 1. doi: 10.1016/j.cvfa.2010.04.005. Bovine Rotavirus & Coronavirus Vaccine: Vaccine info: Killed Virus. ScourGuard® 4K is vaccine for healthy, pregnant cows and heifers as an aid in preventing diarrhea in their calves caused by bovine rotavirus (serotypes G6 and G10), bovine coronavirus, and enterotoxigenic strains of Escherichia coli.
Calf Scours Management: The health- and life-threatening causes of diarrhea in calves are commonly from a list of infectious pathogens that are shed at low levels by individuals in virtually any group of bovines. Most are viral or protozoal, and some are bacterial. These pathogens are picked up by calves, amplified, and shed at much higher levels into the environment, mainly in feces. Calves born later in the calving season are often born into environments that have much higher levels of these pathogens present than the earliest calves experienced, and as a result, the later-born calves are at higher risk of getting sick. One method that many producers have been successfully implementing in Nebraska for years to break this chain of transmission is called Sandhills Calving. This method involves keeping cow-calf pairs with only calves born in the same one- to two-week period together until the youngest calves are at least a month old. This prevents amplification of pathogens from continuing to accelerate and provides a fresh start for each one- to two-week batch of calves. When cow-calf pairs are in pens in the spring, the calves need a clean, dry place to lie down. Usually, this needs to be somewhere that the cows can't get into, and it needs to be out of the wind. Shelter can be beneficial if the ventilation is adequate. Sometimes it can be as simple as an electric fence stretched diagonally across the corners of the pen, raised high so calves can go freely underneath, but the cows are fenced out. This allows calves an escape where they can lay in some clean dry straw.
Bovine Leukemia Virus (BLV): Transferred from blood to blood. There is no vaccine for BLV. There is no cure.
If a cow is BLV positive it is positive for life.
Milk from positive cows is not proven to affect humans but they think it could possibly be linked to lung and breast cancer.
In the U.S. recent surveys indicate close to 90% of dairies and 40% of beef operations have cattle that test seropositive for BLV. Prevention is the only way to control this disease. Eliminate the transfer of blood from infected animals to healthy animals to prevent the spread of this virus. Avoid blood contamination when working cattle or artificially inseminating (AI) cows. And control biting flies. There are three main clinical outcomes in cattle infected with BLV:
- Up to 5% of infected cattle will develop full clinical manifestation of the disease: Lymphosarcoma (fatal).
- About 30% of BLV-infected cattle develop Persistent Lymphocytosis (PL) a benign condition, however, these carrier cows may serve as a reservoir of infection.
- About 65% of exposed cattle will remain asymptomatic, i.e. show no outward signs of disease however sub-clinically infected animals have lowered production, fertility & longevity.
The most commonly recommended BLV eradication protocol is as follows:
- identify infected animals using a serologic test
- cull seropositive animals immediately
- retest the herd in 30–60 days
- repeat testing and cull until the entire herd tests negative
- Testing is then repeated every 6 months. The herd is declared free when there have been no positive tests for 2 years. Additions to the herd should have 2 negative tests 60 and 30 days before arrival.
Bovine Respiratory Disease complex (BRD), AKA Shipping Fever; Dairy Calf Pneumonia or Summer Pneumonia in beef calves; Possibly the most devastating disease of the US cattle population. BRD is a respiratory disease complex caused by a variety of pathogens; viral, bacterial & parasitic, in various combinations, often brought on by stress. BRD affects the lower respiratory tract (lungs--pneumonia) or upper respiratory tract (rhinitis--tracheitis--bronchitis). These contagious viral diseases are widespread, and all herds should be vaccinated annually, usually 30 days prior to breeding with IBR-PI3-BVD-BRSV + Adenovirus vaccine.
BRD in Calves: Reduce stress.
Vaccinate calves 30 days before expected stress (weaning, shipping, exhibition, close confinement)
WHEN to TREAT:
Calf Respiratory Scoring Chart
total respiratory score is
1-4: watch
> 5: treat |
- Infectious Bovine Rhinotracheitis (rednose) (IBR)
agent: Bovine Herpes Virus 1 (BVR-1), produces 3 viral diseases:
• Infectious Bovine Rhinotracheitis (IBR) and
• Infectious Pustular Vulvovaginitis (IPV) in cows
• Infectious Balanoposthitis in bulls
(both exhibited by red and ulcerized genital mucosa)
- Parainfluenza-3 (PI3)
- Bovine Viral Diarrhea Types I and II (BVD)
- Bovine Respiratory Syncytial Virus (BRSV)
- Adenovirus
BRD viruses, especially in Shipping fever, are accompanied by a variety of bacteria (the 4 most common are Pasteurella multocida, Mannheimia haemolytica, Mycoplasma bovis and Histophilus somni--formerly known as Haemophilus somnus). BRD calf scours (calf diarrhea) causes as much financial loss to cow-calf producers as any disease on the farm. Research indicates that many scour cases directly relate to lack of colostrum intake by the newborn calf. A calf that is well mothered and consumes enough (1 to 2 quarts in standard breeds) colostrum in the first 6 hours after birth absorbs a healthy level of antibodies and is far less susceptible to pneumonia, scours and other calfhood diseases such as coccidiosis, etc.
Treatment of symptoms: antibiotics & sulfas, supportive anti-inflammatories, oral rehydration fluids.
Prevention: Vaccinate pregnant cows annually 3–4 weeks prepartum to improve the quality of colostral antibodies.
Brucellosis (Brucella abortus). Zoonotic, reportable disease. RB51 Bangs vaccine is administered by a vet and given to heifers one time between 412 mos of age. Bangs vaccinating before selling breeding heifers over state lines was a common practice out west, but now, the nation is at a crossroads regarding brucellosis. Over the past century, this disease has affected both animal and human health, food safety, international trade, and state and federal regulatory policies. After more than 60 years of eradication efforts and government expenditure of several billion dollars, brucellosis has been nearly eliminated from USA's cattle herds. The last remaining reservoir of brucellosis is in free ranging elk and bison in the Greater Yellowstone Area. Current vaccine and diagnostic technologies to eliminate this disease in free ranging elk and bison have so far been inadequate.
Cancer Eye. Bovine ocular neoplasia includes a variety
of benign and malignant skin tumors of the eyeball and eyelids. Cancer
eye mostly affects cattle that have non-pigmented skin around the eye
(common in Herefords). The peak age for cancer eye is between 7 and
8 years of age. Cancer Eye can be managed by culling affected animals,
and selecting cattle with pigment around their eyes.
Clostridial Disease complex. Prevention: 8-way vaccination prevents clostridial infections that cause Blackleg, Lockjaw (bovine tetanus), Black disease, Red Water disease, malignant edema, gas gangrene, enteritis, enterotoxemia, & other causes of sudden death. Agent: widespread bacteria, in soil & wind, etc. Infection usually results from stress such as unsanitary conditions, crowding, and compromised immunity. Clostridial infections can occur sporadically in herds; and in general, carry a very poor prognosis--the first sign of illness may be sudden death. Because treatment success is rare, emphasis is placed on preventive measures. Cattle should be vaccinated annually with 7-way or 8-way in spring, or in calves, 30 days prior to stress (close contact, branding, castration etc).
 Foot
and Mouth Disease (FMD) United States eradicated FMD disease by 1929. Elsewhere, FMD is a worldwide concern as it can spread
quickly and cause significant economic loss. It is a severe and highly contagious
viral disease that causes illness in cattle and other animals with cloven
hooves. It is caused by one of the smallest disease producing viruses
known. There are 7 known types
and more than 60 subtypes of the FMD virus. Immunity to one type does
not protect an animal against other types or subtypes. Here, APHIS works
to prevent FMD from reentering the country. FMD has serious impacts
on livestock trade—a single detection of FMD would likely stop
international trade completely for a period of time. Since the disease
can spread widely and rapidly and has grave economic consequences, FMD
is one of the animal diseases livestock owners dread most. To help prevent
its resurgence in USA, watch for excessive salivation & lameness
in your herd. When traveling outside the United States, make sure that
you do not bring back prohibited animal products or other at-risk materials. Here is the pdf of the European Union checklist used to accept collection facilities that apply to export bovine semen to EU (FMD is the only disease mentioned by name in this document).
Foot
and Mouth Disease (FMD) United States eradicated FMD disease by 1929. Elsewhere, FMD is a worldwide concern as it can spread
quickly and cause significant economic loss. It is a severe and highly contagious
viral disease that causes illness in cattle and other animals with cloven
hooves. It is caused by one of the smallest disease producing viruses
known. There are 7 known types
and more than 60 subtypes of the FMD virus. Immunity to one type does
not protect an animal against other types or subtypes. Here, APHIS works
to prevent FMD from reentering the country. FMD has serious impacts
on livestock trade—a single detection of FMD would likely stop
international trade completely for a period of time. Since the disease
can spread widely and rapidly and has grave economic consequences, FMD
is one of the animal diseases livestock owners dread most. To help prevent
its resurgence in USA, watch for excessive salivation & lameness
in your herd. When traveling outside the United States, make sure that
you do not bring back prohibited animal products or other at-risk materials. Here is the pdf of the European Union checklist used to accept collection facilities that apply to export bovine semen to EU (FMD is the only disease mentioned by name in this document).
 Footrot,
or infectious pododermatitis, is a hoof infection commonly found in
sheep, goats, and cattle. As the name suggests, it rots away the foot
of the animal, specifically the area between the two toes of the affected
animal. It is extremely painful and it is contagious. Fusobacterium
necrophorum and Bacteroides melaninogenicus are the predominant bacteria
isolated from footrot. Footrot occurs in cattle of all ages, but it
is most common in adults. The disease is seen year-round, but there
is increased incidence in wet summer and fall months. Footrot,
or infectious pododermatitis, is a hoof infection commonly found in
sheep, goats, and cattle. As the name suggests, it rots away the foot
of the animal, specifically the area between the two toes of the affected
animal. It is extremely painful and it is contagious. Fusobacterium
necrophorum and Bacteroides melaninogenicus are the predominant bacteria
isolated from footrot. Footrot occurs in cattle of all ages, but it
is most common in adults. The disease is seen year-round, but there
is increased incidence in wet summer and fall months.
Grass Tetany is a serious, often fatal metabolic disorder
characterized by low levels of magnesium in the blood serum of cattle.
It is also called grass staggers and wheat pasture poisoning. It primarily
affects older cows nursing calves less than two months old, but it may
also occur in young or dry cows and growing calves. It happens most
frequently when cattle are grazing succulent, immature grass and often
affects the best cows in the herd. The prevention of grass tetany depends
largely on avoiding conditions that cause it. Graze less susceptible
animals (steers, heifers, dry cows, and cows with calves over 4 months
old) on higher risk pastures. In areas where grass tetany is a frequent
occurrence, feed cows supplemental magnesium.
Johne's disease in cattle, (Paratuberculosis) is caused by M. avium subspecies paratuberculosis (MAP), a bacterium related to tuberculosis. Johne's disease affects ruminants, including cattle, sheep, and goats. This chronic intestinal disease is distributed worldwide and takes a heavy economic toll on animal producers. No vaccine [in USA], no cure. At least 8% of United States beef herds are believed to be MAP-infected. In dairy cattle, from 65% of small herds, and up to 95% of large herds in United States are believed to be MAP-infected. The dairy industry incurs substantial economic losses due to reduced milk production, premature culling, and reduced slaughter value (Raizman et al., 2009). It takes years for clinical signs to appear in animals after initial infection. The bacterium is shed in high numbers in the feces during this clinical phase of disease. Transmission is by ingestion of the bacterium while grazing on pastures contaminated by this shedding process. Milk, passed from the infected dam to the daughter, has also been shown as a transmission route (Stabel, 2008). Johne's disease has been reported in almost all countries around the world. Controlling Johne's disease; and Johne's Disease [Cornell University].
Leptospirosis (Lepto) is caused by the spiral-shaped bacteria Leptospira, which has more than 400 subclassifications called serovars. It is a worldwide zoonotic infectious
bacterial disease of many animal species causing abortion, stillbirths,
milk loss and reproductive inefficiency. Cattle, sheep and goats can
get infected. The disease does not normally manifest in sheep--but they
are major carriers. In cattle, after the first phase of the infection,
the bacteria localize in the uterus and sex glands and in the kidneys.
The early symptoms of infection are often so brief that in breeding
cattle, subclinical or chronic infection may manifest first as abortion
and lowered fertility. Estimates of leptospiral infection in a sample
of US dairies and beef cow-calf operations indicated that the overall
herd infection prevalence was up to 50% (Grooms, 2004, Bolin 2003).
Bovine leptospirosis vaccines available in the USA and Canada contain
leptospiral serovars Pomona, Grippotyphosa, Canicola, Icterohaemorrhagiae,
and Hardjo. These vaccines provide good protection against disease caused
by each of these serovars, with the possible exception of serovar Hardjo.
Sheep can serve as a maintenance host for serovar Hardjo and therefore
spread infection to cattle. Risk factors for Hardjo infection in cattle
include co-grazing with sheep, open herds, access to contaminated water
sources, and use of natural breeding. Serovar hardjo has the ability
to colonize and persist in the genital tract of infected cows and especially
bulls. If a primary goal of a vaccination program is protection of cattle
against Hardjo, care should be taken in selection of a vaccine product.
In general, annual vaccination of all cattle in a closed herd or low incidence area, or twice-yearly vaccination in an open herd or high
incidence area, is the most effective approach to control. Antibiotic
treatment or combined antibiotic and vaccination therapy of cow herds
suffering from active Leptospira-infection have been shown to have some
success. Eradication may be attained in about 5-6 years in a closed
herd. Most Lepto vaccines are a 5-way + Vibrio combination.

Listeriosis is a disease of the central nervous system, caused by the bacterium
Listeria moncytogenes. This bacterium can live almost anywhere--in soil,
manure piles, and grass. Listeriosis is common in cattle, sheep and
goats and can occur in pigs, dogs, and cats, some wild animals, and
humans. Animals infected with Listeria can show signs restlessness,
loss of appetite, fever and nervous system disorders. Although not seen
in every case, the most notable symptom gives this disease its nickname, "Circling Disease." Cattle with listeriosis are often seen walking in
circles. Other, more subtle symptoms include uncoordinated movements,
leaning against objects, and progressive paralysis. Death can occur
within 2 to 3 days after the onset of symptoms, but cattle can survive
for up to 2 weeks with the disease. Healthy animals are not usually
affected by Listeria. Cattle with lowered resistance to disease are
prime candidates for listeriosis. Recognition of symptoms is important
for successful treatment. Most animals will recover if treated with
a broad spectrum antibiotic started early. Diseased cattle should be
separated from healthy cattle and placed on a prolonged therapy program.
In herds of valuable cattle, it may be advantageous to treat the whole
herd. Vaccines are not available in the U.S.
Lumpy Jaw. Actinomycosis or lumpy jaw produces immovable
hard swellings on the upper and lower jawbones of cattle, commonly at
the central molar level. It is caused by an anaerobic micro-organism,
Actinomyces bovis. The bacterium invades tissue through breaks in the
lining of the mouth caused by eating rough forage. The tumor-like swellings
develop slowly and may take several months to reach a noticeable size.
The most common treatments are iodine therapy or tetracyclines. Treatment
is often ineffective. If the disease is detected early, it may be better
to cull the animal while it is still in good condition. Only the head
should be condemned by meat inspectors, unless the lesions have spread
elsewhere in the body.
Mad Cow Disease, or Bovine
Spongiform Encephalopathy (BSE), are progressive and fatal
neurologic diseases of cattle with no cure or vaccine. BSE is a reportable
disease. Due to its etiology, Mad Cow Disease is not addressed in most
herd health programs. Included here FYI, and to shed some understanding
as to why cattle are not imported or exported between USA and UK or
Europe.
IMPORTANT: BSE exists in two forms which are believed to be biologically
distinct:
- C-type Classical (Mad Cow
Disease, zoonotic; linked to vCJD disease in humans, not found
in USA)
- L-type ATypical (a spontaneous
disease in older cows that occurs worldwide, but is very rare)
H-type ATypical (a spontaneous disease in older cows that occurs worldwide, but is very rare)
The primary cause & source
of infection for classical BSE is feed contaminated with the infectious
prion agent, such as meat-and-bone meal containing protein derived from
rendered infected cattle; the highest risk tissue comes from the brain
and spinal cord. A variant of Creutzfeldt-Jakob disease (vCJD) in people
was linked to exposure to the classical BSE in cattle. BSE was first
diagnosed in 1986 in the United Kingdom, which has had the vast majority
of cases worldwide. However, the disease has been detected in many other
countries, including six cases in the United States from 2003 to 2012.
Of the six U.S. cases, the first in 2003 was the only case of classical
BSE, found in a cow imported from Canada. The rest were atypical BSE.
The 2 atypical BSE forms, L-type and H-type, occur rarely and spontaneously
(no known cause), in cattle around the world; usually eight years of
age or older. Read about DNA testing for resistance to BSE in cattle, here.


Malignant
Catarrhal Fever (MCF) is a generally fatal
disease of cattle, bison, true buffalo species, and deer. No vaccination,
no cure. It is caused by viruses belonging to the Herpesvirus family.
MCF occurs worldwide and is a serious problem in North America most
especially for bison. MCF in bison & cattle is caused by a virus
called ovine herpesvirus-2 (OvHV-2). Sheep infected with OvHV-2 are
the principal source of MCF outbreaks in bison and cattle. The virus
comes from sheep by contact, but does not spread from cow-to-cow by
contact. Almost all sheep are carriers (over 98%), but the virus does
not cause illness in sheep.
Mastitis caused by Staphylococcus aureus (S. aureus infection). There are estimates that 80-100% of all herds have at least some S. aureus mastitis, with from 5 to 10% of cows infected. S. aureus organisms colonize teat ends and/or teat lesions. Spread of infection can occur through milkers’ hands, washcloths, teat cup liners, and flies. During milking, irregular vacuum fluctuations can force bacteria up into the teat canal, leading to the potential for new infection. Staph mastitis treatment has a low success rate. Control measures are best gained through prevention of new infections and culling of infected animals. Testing is important when bringing in new cattle. There is a 2020 study in Chinese Holsteins that indicate there may be a genetic resistance v. susceptibility component.
Neosporosis Neospora caninum is a microscopic protozoan
parasite
whose natural host is dogs and wild canids, such as coyotes.
Try to keep dogs access to feed sources
limited. Infection occurs when cattle inadvertently consume feces from these canids. Once cows in a herd become infected, they pass the infection along to their calves while the calf is still in the cow's uterus. While abortion may occur, the majority of infected calves are normal at birth. Stillborn calves and weak or paralyzed calves that may have convulsions are also seen. 80% of live calves born of infected cows are themselves infected. Infected females kept as replacements are more likely to abort and/ or give birth to infected calves. Infected cattle are considered infected for life though their risk of abortion decreases with each calving. A killed vaccine is available. The vaccine is not useful in cows that are already infected but seems to help prevent new infections in uninfected cows.
New
World Screwworm of interest only to herd owners who live
in or visit the Florida Keys.
Pinkeye (Infectious
B Keratoconjunctivitis) (IBK) bacteria. It is known to occur at all
seasons of the year and in all breeds of cattle. There are treatments
such as antibiotic & anesthetic spray for the eyes, etc., while
a control program should include measures taken to reduce sources of
initial eye irritation. This may be fly control, clipping pastures,
providing shade, or using breeds less prone to pinkeye, and vaccinating
for pinkeye prior to fly season.

Q fever (Query
fever) is a worldwide (except New Zealand) zoonotic disease.
Caused by a bacteria carried by livestock, Query (Q) fever is a rare disease first discovered in 1947 and is found mostly in dry, dusty areas of California and the Southwest.
Like anaplasmosis,
it is caused by another parasitic rickettsial type bacteria, Coxiella
burnetii, and it lives inside White Blood Cells. Infected cattle, sheep,
or goats serve as a reservoir for C. burnetii bacteria, and are the
primary hosts implicated in human outbreaks. Infected cattle are usually
sub-clinical, however, infected herds have increased incidence of abortion,
stillbirth and weak calves, lowered fertility, lower milk yield, metritis
or chronic mastitis and possibly even respiratory disorders and cardiac
failure. Veterinarians, meat processing plant (abattoir) workers, and
dairy and livestock farmers who work with pregnant cattle, sheep or
goats are most at risk for exposure to Q fever. It is contracted from
contact with excretions such as raw milk, urine, feces and afterbirth
from infected animals. The C. burnetii bacterium remains viable for
a long time in soil. Most human infections are believed to be caused
by inhalation of contaminated barnyard dust. A 2019 survey reported by Iowa DoA indicated that 82% of cows in some California dairies were seropositive, as well as 78% of coyotes, 55% of foxes, 53% of brush rabbits, and 22% of deer in Northern California. Clinical human Q fever
disease is treated with antibiotics, typically tetracyclines. There
is little evidence that antibiotic treatment in animals provides any
significant benefit.
Ringworm is a transmissible infectious skin disease
caused most often by Trichophyton verrucosum, a spore forming fungi.
It occurs in all species of mammals including cattle and man. Although
unsightly, fungal infections cause little damage or economic loss. Ringworm
fungi spores can remain alive for years in a dry environment. Direct
contact with infected animals is the most common method of spreading
the infection. Ringworm is most frequent on the head and neck, but it
may be found over the entire body in severe cases. Infection spreads
from the center outwards and resulting in a circular lesion. Scabs fall
from older lesions leaving a ring with a hairless area in the center.
Hence, the name ringworm. Ringworm will usually cure itself without
treatment. Common treatments include topical application of a 2% solution
of iodine, thiabendazole paste or any good fungicide. Cattle usually
become immune to ringworm after the first instance of it.
Salmonella
Dublin is a bacterial disease that can cause pneumonia,
diarrhea and reproductive losses, and fever or swelling joints in calves.
It is a fairly recent newcomer to U.S. dairy herds. Over the past 20
years, it has slowly crept into every major dairy area in the U.S. Once
infected, of the calves that don’t die from it, a proportion (5-20%)
will become carriers for life and shed the bacteria intermittently in
feces, colostrum, milk or semen. Antibiotic treatments can knock back
acute infections, but might not rid the animal of the disease. And while
a vaccine is available for use in calves, later tests can’t differentiate
between a vaccinated and an infected animal. Lab tests for this salmonella
are most accurate when used on calves 3 to 10 months of age. Salmonella
Dublin is a zoonotic disease, meaning it can be transferred to humans.
It is killed by pasteurization.
Trichomoniasis (Trich, an STD) is a venereal disease of cattle
that causes infertility and occasional abortions in cows, caused by
Trichomonas fetus, a small motile protozoan that lives in the reproductive
tracts of cattle.
• Trich organism infects the genital tract
of the bull and is transmitted to the cow during breeding
• Trich can be confirmed microscopically
• Infected bulls are normally carriers for
life
• Clean bulls can be infected by breeding
“dirty” cows
• Prevention:
• vaccinate healthy herds annually
prior to breeding
• use virgin bulls
• use certified frozen semen
Tuberculosis or Bovine TB - caused by the bacteria, Mycobacterium bovis; no vaccination, no practical cure. Zoonotic. Tuberculosis is similar to brucellosis, another highly contagious disease carried by cattle. Both TB & Bangs are often spread to humans by infected placental material during calving. Unpasteurized milk from infected dairy cows can also infect humans. M. bovis TB infections in United States cattle herds are not common, however, M. bovis is endemic in white-tailed deer in parts of Michigan and Minnesota. Also, there are sporadic imports of the disease coming up from Mexico. To avoid the chances of cattle being infected by tuberculosis or brucellosis, ensure cattle are bred and brought in from a reliable herd. Do not borrow or lend calving equipment. Isolate or cull infected animals.
Vesicular Stomatitis Virus (VSV) - Excessive salivation,
blister-like lesions on the lips, gums, tongue, dental pad, nostrils,
coronary band, prepuce, vulva, and teats, with fever, are usually the
first signs of VS. The blisters swell and break, which causes oral pain
and discomfort and reluctance to eat or drink. Lameness and severe weight
loss may follow. Cows that suffer from teat lesions can develop mastitis.
Some infected cattle can appear subclinical, other than going off their
feed. VS is zoonotic and is recognized internationally as a reportable
disease. While vesicular stomatitis does not generally cause animals
to die, there are serious economic and regulatory repercussions associated
with the diagnosis. The Southwestern and Western United States have
experienced a number of VSV outbreaks, usually during warmer months,
often along waterways. Surveillance is conducted by the State Departments
of Agriculture in conjunction with USDA - APHIS - Veterinary Services.
Veterinarians examine all animals involved in shows, exhibitions, races,
and interstate or international movement.
Vibriosis (Campylobacter) (an STD) is a venereal disease
most often spread by infected bulls when they breed susceptible cows.
It is considered to be the most significant cause of infertility in
cattle. Diagnosis is confirmed by culture of the causative organism
from cervical mucus or from an aborted fetus. Vaccination involves two
injections, 4-6 weeks apart in the first year, with a single dose administered
each year thereafter. Vaccination should be completed 4 weeks prior
to breeding. Lepto & Vibrio are often included in the same vaccine.
Most A.I. organizations test frozen semen to assure that it is free
of vibriosis and trichomoniasis. The use of AI helps in prevention because
frozen semen is treated with antibiotics to eliminate Campylobacteriosis
disease organisms.
Warts in cattle are caused by the contagious papilloma
virus. Four types of the virus are known to produce warts on cattle.
Calves are most susceptible. Few warts are seen in cattle over 2 years
of age. Warts appear 1 to 6 months after infection with the virus; and
not all animals carrying the virus will have warts. It can be transmitted
from the unapparent carrier to the susceptible calf. Warts are usually
more of a cosmetic problem than anything. Warts usually shrink and drop
off after a few months. This spontaneous resistance & recovery is
probably the basis for the alleged effectiveness of many home remedies.
Warts can also be removed surgically with sharp scissors or a side cutter.
If there is a severe outbreat in the herd an autogenous vaccine can
be prepared from chemically treated warts taken from animals in the
affected herd. The autogenous vaccine is more apt to have the strain
or type of papillomavirus causing the wart problem in the herd than
commercially prepared vaccines.
Wooden tongue is an infection caused by a rod-shaped
bacterium, Actinobacillus lignieresii, which lives only in the presence
of oxygen. Wooden tongue occurs almost entirely in soft tissue with
the tongue and lymph nodes of the head most often affected. The bacteria
invades tissue through breaks in the lining of the mouth. Any rough
feed can cause mouth abrasions which can lead to infection. The disease
starts suddenly with the tongue becoming hard, swollen and painful.
Affected animals drool saliva and may appear to be chewing gently. The
tongue often protrudes between the lips and nodules and ulcers may be
observed on the tongue. They are unable to eat or drink and rapidly
lose condition. The disease is progressive and often fatal unless treated.
It is important to begin treatment early, which is usually successful,
while advanced cases may fail to respond. The most common treatments
are iodine therapy or tetracyclines. Advanced cases may require surgical
drainage and irrigation with iodine solution for several days. Treated
animals should be observed regularly, as relapses can occur.
|

![]()
![]()
![]()
![]()






 Footrot,
or infectious pododermatitis, is a hoof infection commonly found in
sheep, goats, and cattle. As the name suggests, it rots away the foot
of the animal, specifically the area between the two toes of the affected
animal. It is extremely painful and it is contagious. Fusobacterium
necrophorum and Bacteroides melaninogenicus are the predominant bacteria
isolated from footrot. Footrot occurs in cattle of all ages, but it
is most common in adults. The disease is seen year-round, but there
is increased incidence in wet summer and fall months.
Footrot,
or infectious pododermatitis, is a hoof infection commonly found in
sheep, goats, and cattle. As the name suggests, it rots away the foot
of the animal, specifically the area between the two toes of the affected
animal. It is extremely painful and it is contagious. Fusobacterium
necrophorum and Bacteroides melaninogenicus are the predominant bacteria
isolated from footrot. Footrot occurs in cattle of all ages, but it
is most common in adults. The disease is seen year-round, but there
is increased incidence in wet summer and fall months.

